
Abscesses Explained: Skin, Dental, Internal, and General
An abscess can be uncomfortable, painful, and unsettling, especially when you’re not sure what’s causing it or how serious it might be.
Many people ignore early signs, try to manage symptoms at home, or confuse an abscess with less serious conditions like cysts or skin irritation. That delay often leads to worsening infection, more pain, and more complex treatment than necessary.
Understanding what an abscess is, how it forms, and how it should be treated makes a real difference in how quickly you recover and how safely the problem is managed.
In this guide, you’ll find clear, patient-focused explanations of what abscesses are, what they look like, the different types (skin, dental, and internal), common symptoms and causes, available treatment options, and when medical care becomes necessary. The goal is to give you clarity, reduce uncertainty, and help you recognize when it’s time to seek professional care.
To ensure greater reliability in the content of this article, we interviewed Dr. Yeh, a member of the American Association of Oral and Maxillofacial Surgeons. Enjoy reading!
What is the medical definition of “abscess”?
“An abscess is defined medically as a localized collection of pus that develops within the body's tissues, organs, or enclosed spaces. This formation is the consequence of infection and the body's inflammatory response.” — Dr. Yeh.
It occurs when the immune system isolates invading bacteria or other pathogens, creating an area where fluid, dead cells, and immune cells are trapped to contain the infection.
According to the U.S. National Library of Medicine’s MedlinePlus, an abscess is described as “a collection of pus in any part of the body” that typically causes swelling and inflammation around the affected area. The National Cancer Institute’s medical dictionary similarly defines an abscess as “an enclosed collection of pus in tissues, organs, or confined spaces in the body,” typically indicating the presence of an infection.
Medically, the term reflects not just the pus itself, but the immune response that walls off an infection, which is why abscesses often appear as swollen, painful, and warm areas where white blood cells have concentrated to fight microbes. (MedlinePlus)
In everyday language, when people say “abscess,” they’re usually referring to this pocket of infected pus and inflamed tissue that can occur either just under the skin or deep within the body.
What do abscesses look like?
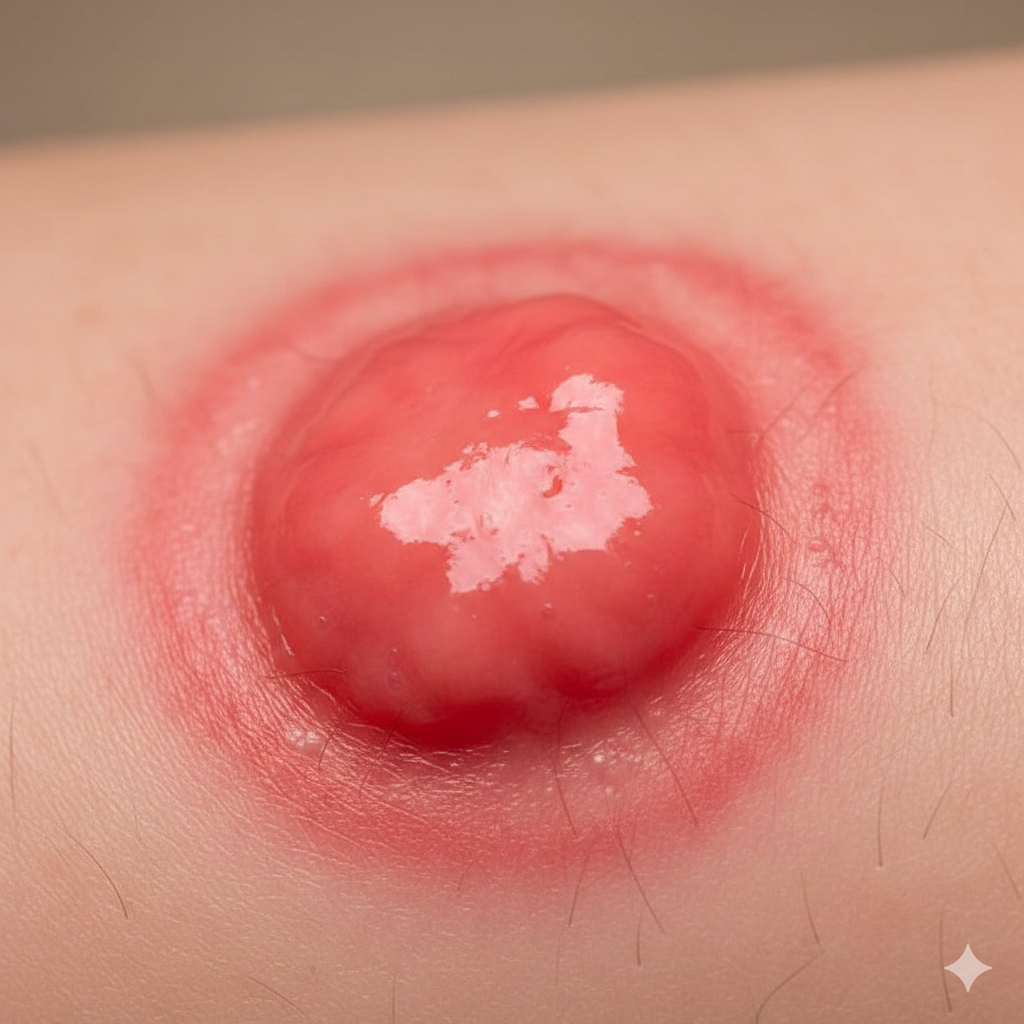
The appearance of an abscess depends on where it forms, but most share a few recognizable features.
A typical abscess looks like a swollen, raised area that may appear red, inflamed, and irritated. The skin or tissue around it often feels warm and tender, and the area may feel firm or tight to the touch.
As abscesses develop, they can form a visible center or “head” where pus collects beneath the surface. This area may look pale, white, or yellowish, especially in skin abscesses.
In dental abscesses, the swelling may appear in the gums, jaw, face, or neck, sometimes without a visible surface opening.
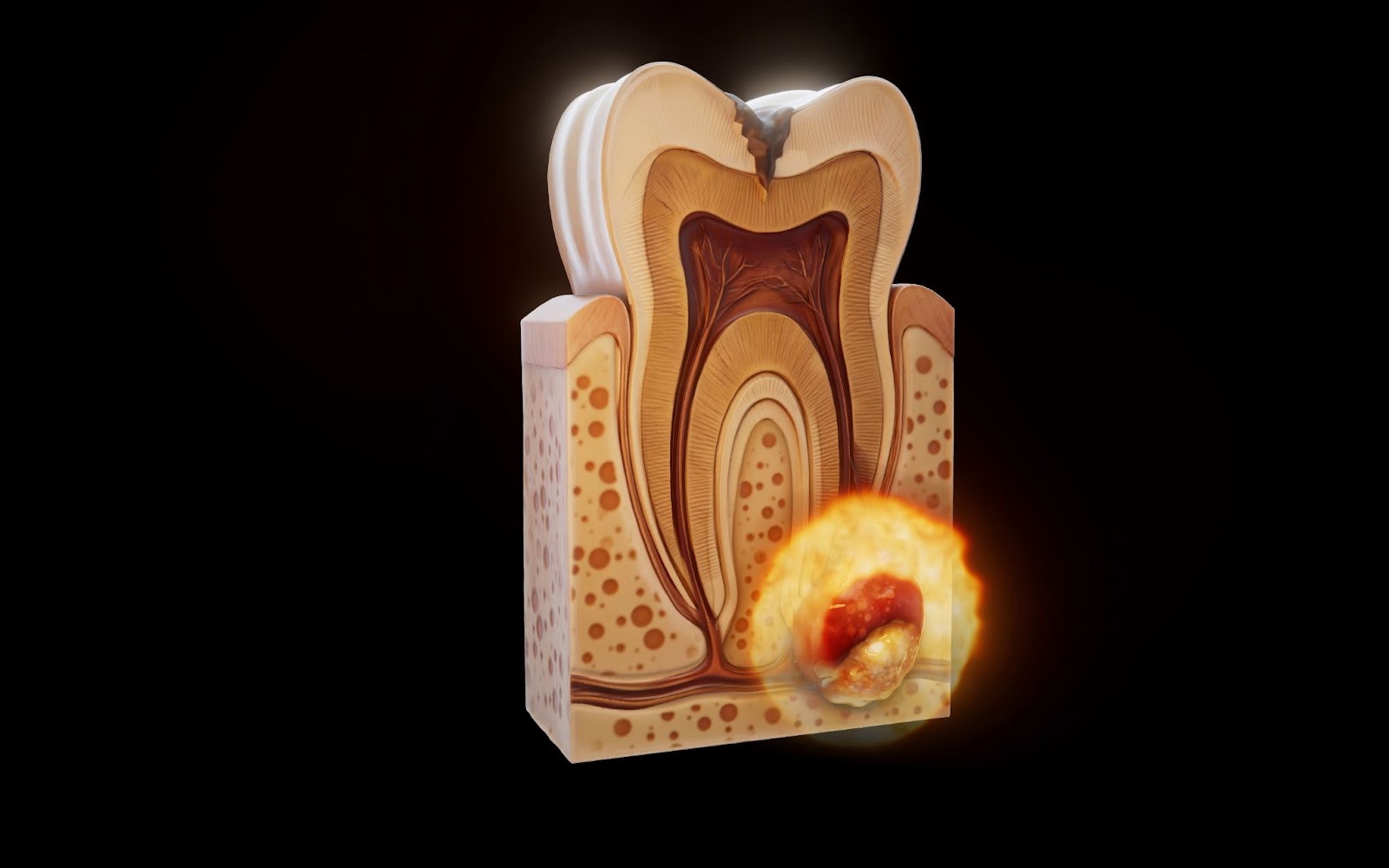
Not all abscesses are easy to see. Internal abscesses can develop deep in the body, where there may be no visible swelling at all. In these cases, signs often show up as pain, pressure, fever, or general illness rather than a visible lump.
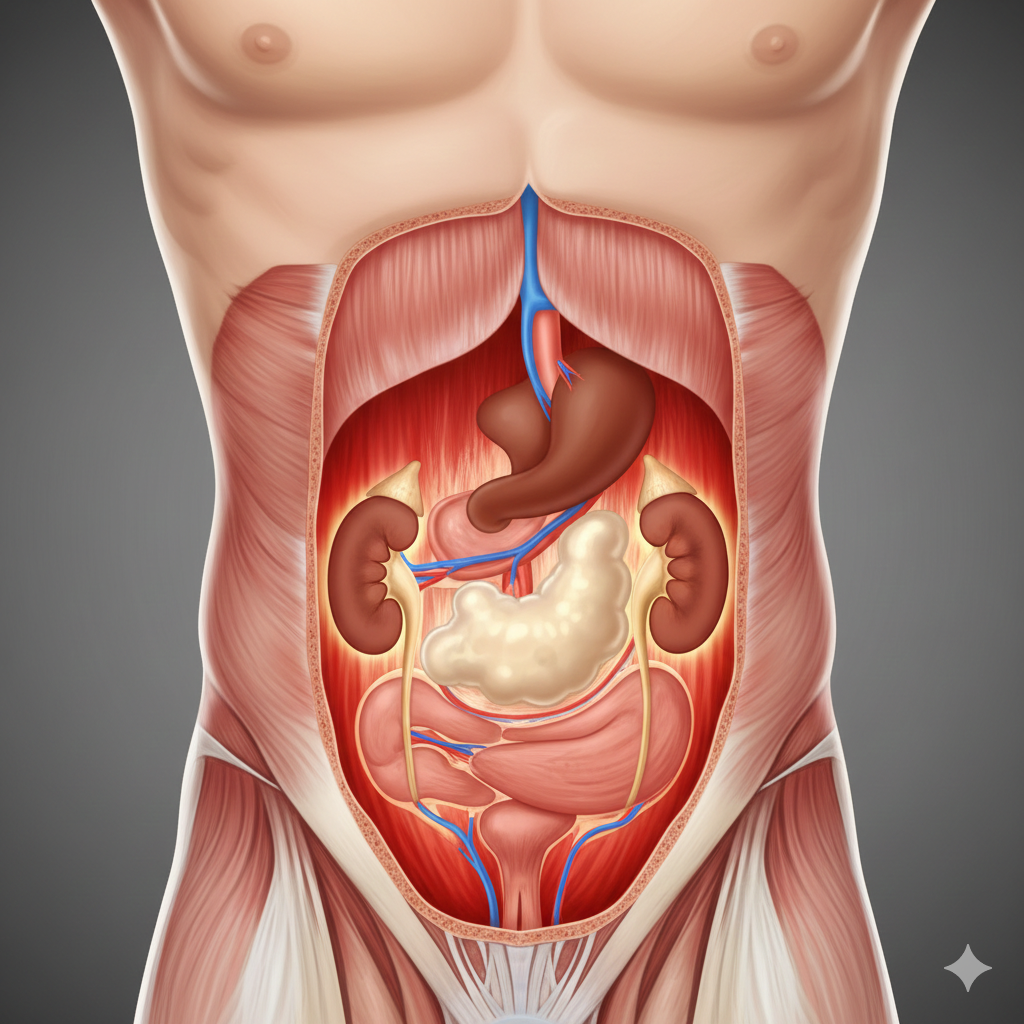
What matters most is not just how an abscess looks, but how it feels and behaves. Increasing pain, spreading redness, warmth, swelling, or drainage are signs that the infection is active and the area needs medical attention.
Abscess vs cyst
Dr. Yeh comments on the differences between abscesses and cysts:
“They can look similar, but they are very different conditions and require different types of care. One key difference is inflammation. Abscesses usually show clear signs of infection, such as redness, heat, pain, and sometimes fever. Cysts typically do not cause these symptoms unless they become secondarily infected, at which point they may start to resemble an abscess.”
An abscess is caused by an infection. It forms when bacteria enter the body and trigger an immune response, leading to a pocket of pus made up of bacteria, dead tissue, and immune cells. Abscesses are usually painful, warm, swollen, and inflamed, and they often worsen without proper treatment because the infection continues to spread inside the tissue.
A cyst, on the other hand, is a closed sac of fluid, air, or other material that is not usually caused by infection. Many cysts develop from blocked glands, hair follicles, or normal tissue changes. They are often slow-growing, firm, and painless, and the skin over a cyst typically looks normal unless it becomes infected.
These definitions go in line with Hecht and Cobb, saying “a cyst is a sac or cavity that may be filled with pus, semi-solid material, or air. It doesn’t usually cause pain until it gets large. An abscess is a painful, red infection that’s filled with pus.”
Distinguishing them matters because treatment is different. Abscesses often require medical drainage and antibiotics, while cysts may only need monitoring or simple removal if they cause discomfort or complications.
Types of abscess
Abscesses can form in many areas of the body, but they are usually grouped into a few main categories based on location and cause. Each type behaves differently and may require different treatment approaches.
Skin abscesses
These are the most common types. They form just under the skin when bacteria enter through small cuts, hair follicles, insect bites, or blocked pores. Skin abscesses often appear as red, swollen, painful lumps and may develop a visible head filled with pus. Examples include boils and furuncles.
Dental abscesses
A dental abscess forms when bacteria infect the tooth, gums, or surrounding bone. This can happen due to untreated cavities, gum disease, cracked teeth, or dental trauma. Swelling may appear in the gums, jaw, face, or neck, and pain can range from mild pressure to severe throbbing. These infections can spread if not treated properly.
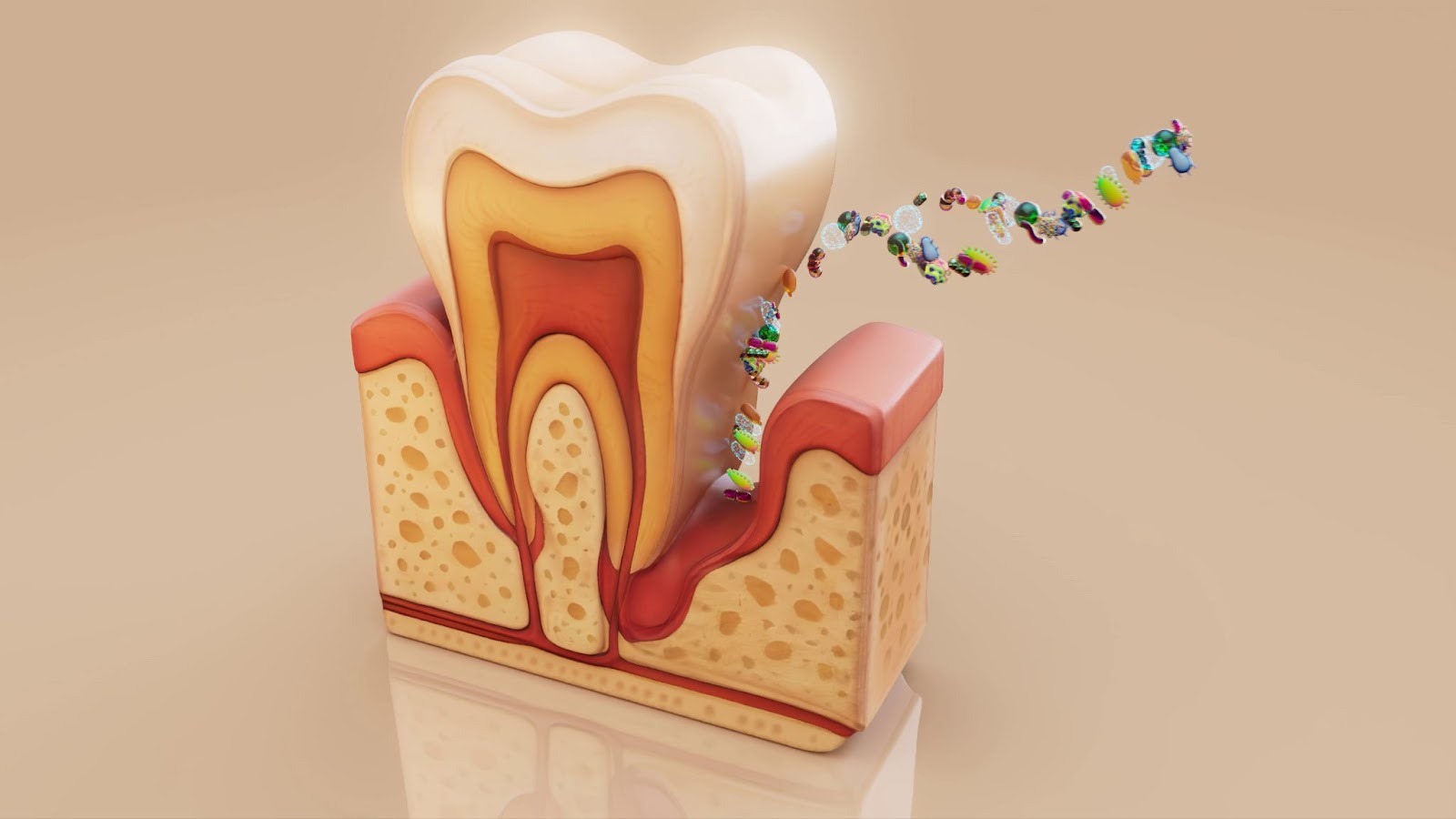
Internal abscesses
Internal abscesses develop inside the body, affecting organs or deep tissues such as the abdomen, lungs, brain, or spine. These are not visible on the surface and often cause symptoms like deep pain, fever, fatigue, and general illness rather than a visible lump. Imaging tests are usually needed to diagnose them.
Peritonsillar and throat abscesses
These form near the tonsils or in the throat area, often as a complication of tonsillitis or throat infections. They can cause difficulty swallowing, voice changes, and swelling in the neck or jaw.
Post-surgical abscesses
These can develop after medical or dental procedures if bacteria enter the tissue during healing. They may appear near surgical sites and are usually associated with increasing pain, swelling, and redness instead of normal healing.
While these abscesses share a common cause (infection), their location determines the symptoms, risks, and treatment options, which is why proper evaluation matters for safe and effective care.
Abscess causes
Abscesses develop when bacteria or other pathogens enter the body and trigger an immune response.
“Your immune system tries to isolate the infection, creating a pocket where pus, dead tissue, and immune cells collect. This process is the body’s way of containing the infection, but it also leads to swelling, pain, and tissue damage if the infection continues.” — Dr. Yeh.
What is the main cause of abscesses?
The most common cause of an abscess is bacterial infection. Bacteria can enter the body through:
- Small cuts or breaks in the skin
- Infected hair follicles
- Dental cavities or gum disease
- Blocked glands or pores
- Surgical wounds or medical procedures
- Trauma to the skin or soft tissue
Once bacteria enter, the body’s immune response creates inflammation and fluid buildup, which leads to abscess formation. In dental cases, untreated tooth decay or gum infection allows bacteria to spread into deeper tissues, forming a localized infection.
Why do I keep getting abscesses?
Repeated abscesses often point to underlying risk factors rather than isolated infections. Common contributors include:
- Weakened immune system, from conditions such as diabetes, autoimmune disorders, or certain medications
- Chronic skin conditions that damage the skin barrier
- Poor circulation, which reduces the body’s ability to fight infection
- Recurrent dental infections, untreated cavities, or gum disease
- Poor wound healing or frequent skin injuries
- Close contact environments, where bacteria spread more easily
In some cases, recurring abscesses may be linked to bacterial colonization on the skin or in the nasal passages, making reinfection more likely. If abscesses keep returning, a medical evaluation is important to identify the underlying cause and reduce the risk of repeated infections and complications.
Abscess symptoms
Abscess symptoms can vary depending on where the infection forms, but most abscesses share a consistent pattern of local and sometimes systemic signs. These symptoms develop as the body responds to infection and inflammation in the affected area.
Common symptoms include:
- Localized pain or tenderness, often worsening over time
- Swelling and redness around the affected area
- Warmth in the surrounding skin or tissue
- A firm or tight feeling under the skin
- Visible pus or drainage in surface abscesses
- Throbbing or pressure-like pain
In dental abscesses, symptoms may also include:
- Gum swelling or a pimple-like bump on the gums
- Jaw, face, or neck swelling
- Sensitivity to hot or cold
- Pain when chewing or biting
- Bad taste in the mouth or foul odor
With internal abscesses, symptoms are often less visible and more systemic, such as:
- Fever or chills
- Fatigue
- General feeling of illness
- Deep or persistent pain
- Nausea or loss of appetite
Symptoms that worsen, spread, or fail to improve are signs that the infection is active and needs medical attention. Early treatment helps prevent complications and limits the risk of the infection spreading to surrounding tissues or the bloodstream. Consult a doctor!
Can an abscess go away on its own?
Some very small abscesses may drain and improve on their own, but this is not the typical or safest outcome.
In most cases, an abscess does not fully resolve without proper treatment because the infection is trapped inside a pocket of tissue. Even if surface swelling decreases, bacteria can remain inside and continue to spread.
When an abscess drains on its own, it may appear to improve temporarily. However, incomplete drainage often leads to recurrence, deeper infection, or worsening inflammation. This is especially true for dental and internal abscesses, which rarely heal without medical care.
Relying on an abscess to resolve without treatment increases the risk of complications, including:
- Spread of infection to the surrounding tissue
- Development of larger or deeper abscesses
- Bloodstream infection
- Chronic or recurring infections
- Tissue damage
Medical evaluation allows the infection to be treated safely through proper drainage, antibiotics when needed, and care that supports healing. Early treatment reduces pain, limits complications, and shortens recovery time.
How do you treat abscesses?
Treatment for an abscess depends on its size, location, severity, and the person’s overall health. The goal is to remove the infection, relieve pressure, and allow the tissue to heal safely. In most cases, treatment involves a combination of drainage, medical care, and infection control.
Medical drainage
The most common and effective treatment is professional drainage. A healthcare provider opens the abscess in a controlled, sterile way to allow the pus to drain completely. This relieves pain, reduces pressure, and removes the source of infection. Proper drainage also lowers the risk of the infection spreading.
Antibiotics
Antibiotics may be prescribed when:
- The infection is spreading
- There is a fever or systemic illness
- The abscess is large or deep
- The immune system is weakened
- The abscess involves high-risk areas (such as the face, jaw, or neck)
Antibiotics alone often do not cure an abscess without drainage because the medication cannot fully penetrate the pocket of pus.
Dental and internal abscess care
Dental abscesses often require treatment of the underlying cause, such as:
- Root canal therapy
- Tooth extraction
- Treatment of gum infection
- Drainage of infected tissue
Internal abscesses usually require imaging, specialist care, and sometimes surgical drainage in a hospital setting.
Supportive care
Supportive treatment may include pain management, wound care, and monitoring for signs of spreading infection. Keeping the area clean and following medical instructions closely supports proper healing.
Treatment should always be guided by a medical professional. Attempting to manage an abscess without proper care increases the risk of complications and recurrence.
FAQ
Are abscesses dangerous?
Abscesses can become dangerous if they are not treated properly. While some are small and localized, others can spread infection into surrounding tissue, the bloodstream, or deeper structures in the body.
On the other hand, according to Dr. Yeh, “dental and internal abscesses carry higher risks because infections in these areas can affect vital systems.”
Early treatment reduces the chance of serious complications.
When should I see a doctor for an abscess?
You should seek medical care if you notice:
- Increasing pain, swelling, or redness
- Fever or chills
- Spreading inflammation
- Drainage with a foul odor
- Facial, jaw, or neck swelling
- Difficulty swallowing or breathing
- An abscess that does not improve
Any abscess that worsens or fails to heal should be evaluated by a medical professional.
Do abscesses always need to be drained?
Most abscesses require drainage to heal properly. Antibiotics alone often cannot fully treat an abscess because medication does not penetrate the pocket of pus effectively. Some very small abscesses may resolve with monitoring, but medical evaluation helps determine the safest approach.
Can I pop or drain an abscess at home?
Draining an abscess at home is not safe. This increases the risk of spreading infection, causing deeper tissue damage, and introducing new bacteria into the area. Improper drainage can also lead to recurrence or serious complications. Abscess drainage should always be done by a trained medical professional in a sterile setting.
What happens if an abscess is left untreated?
An untreated abscess can grow, spread infection to surrounding tissues, and cause systemic illness. Possible complications include bloodstream infection, tissue destruction, chronic infection, and the formation of deeper abscesses. In dental cases, infection can spread into the jaw, neck, and sinuses.
How long does an abscess take to heal?
Healing time depends on the size, location, and treatment method. Small abscesses may improve within days after proper drainage, while larger or deeper abscesses may take weeks to heal fully. Following treatment instructions and attending follow-up care supports proper recovery.
Are abscesses contagious?
The abscess itself is not contagious, but the bacteria causing the infection can spread through direct contact with drainage or contaminated surfaces. Proper hygiene, wound care, and avoiding contact with infected material reduce the risk of transmission.
How can I prevent abscesses?
Prevention focuses on reducing infection risk and supporting immune health:
- Keep skin clean and treat cuts promptly
- Avoid squeezing or picking at skin lesions
- Maintain good oral hygiene and routine dental care
- Manage chronic conditions such as diabetes
- Follow proper wound care after procedures
- Seek early treatment for infections
Consistent care and early intervention lower the risk of abscess formation and recurrence.
Seek Treatment Early
Abscesses are more than just painful swellings. They are active infections that form when bacteria become trapped inside the body, creating pockets of pus and inflammation.
As this guide explained, abscesses can affect the skin, teeth, gums, and internal organs, each with different risks, symptoms, and treatment needs.
Recognizing early signs, understanding the causes, and knowing when to seek care all play an important role in preventing complications and supporting safe recovery. Prompt treatment helps limit the spread of infection, reduces pain, and lowers the risk of long-term damage.
Whether an abscess is small and visible or deep and internal, medical evaluation allows it to be managed properly, with appropriate drainage, treatment of the underlying cause, and supportive care that promotes healing.
If you are dealing with facial swelling, dental pain, signs of infection, or concerns about an abscess, professional evaluation matters. Learn more about available care options and how treatment can help!
Early care protects your health and supports safer, faster recovery!

